Evidence based practice
Legislation
There is often a perception that legislation is used to inhibit practice and manage budgets. Phrases such as ‘we don’t do baths’ and ‘my local authority won’t fund baths’ appear commonplace.
However, legislation should instead be used to guide and assist practice. Through greater knowledge of the legislative content, occupational therapists can ensure recommendations remain cost effective whilst meeting long-term, holistic and client-centred needs.
To do this, therapists must reflect on the relationship between legislation and occupational therapy philosophy; how does it support holistic, client-centred practice with an occupational focus?

Some examples of this include:
Housing Grant, Construction and Regeneration Act (1996)
When determining the need for bathing adaptations, the decision more often than not, focuses on whether a bath or shower will be most suitable to meet the client’s ongoing needs. Knowledge of the legislation is essential to understand what work can be carried out using DFG funding.
For example, the Act states that DFGs can be used for ‘Facilitating access by the disabled occupant to, or providing for the disabled occupant, a room in which there is a bath or shower (or both)’.
Therefore, if an individual required a shower to meet specific hygiene needs but a bath for other aspects of occupational engagement such as play, role reinforcement or relaxation, then this is absolutely justifiable. The same could be used where the therapist needs to support the client and family residing in the same property.
Care Act (2014)
The Care Act was a breakthrough piece of legislation that changed focus from physical health to overall wellbeing for social care provision.
The legislation lists nine wellbeing principles including:
- Personal dignity
- Physical and mental health and emotional wellbeing
- Suitability of living accommodation
Although it does not specifically define wellbeing, you should consider aspects of wellbeing beyond just basic activities of daily living. It recognises that wellbeing includes the person’s need to contribute to society and their ability to have control over their day-to-day life. For professionals, the guidance gives them the authority to think more holistically about what contributes to wellbeing.
The Care Act also states that the client is best placed to judge their own wellbeing needs.
Using the wellbeing agenda within recommendations and clearly evidencing the impact on the client is crucial in determining the outcome.
Chronically Sick & Disabled Person Act (1970)
Although superseded by The Care Act for adults, CSDP remains in place for children.
Section 2 lays out a range of services including “assistance with home adaptations, or the provision of additional facilities designed to secure greater safety, comfort or convenience.” How therapists use the terms safety, comfort and convenience to support recommendations can have a big impact on the outcome.
The Children’s Act
Schedule 2 of the Act requires that Local Authorities provide services to minimise the effect of disabilities on children and give such children the opportunity to lead lives which are as normal as possible.
In the context of bathing, which is widely regarded as a normal daily activity for children in the UK, this means that all children (client and their siblings) have the right to bathe.
Although this is not an exclusive list of legislation, it provides an example of how the specific wording, if known, can be used to actively promote positive change, whilst maintaining the occupational therapy philosophy of client centred, holistic and occupation focused intervention.


Clinical reasoning
Clinical reasoning is the process therapists go through to determine, justify and defend their recommendations. To ensure that the clinical reasoning is robust the therapist must ensure that they have all of the required information about the person, their environment, their meaningful occupations and the most relevant up to date evidence base.
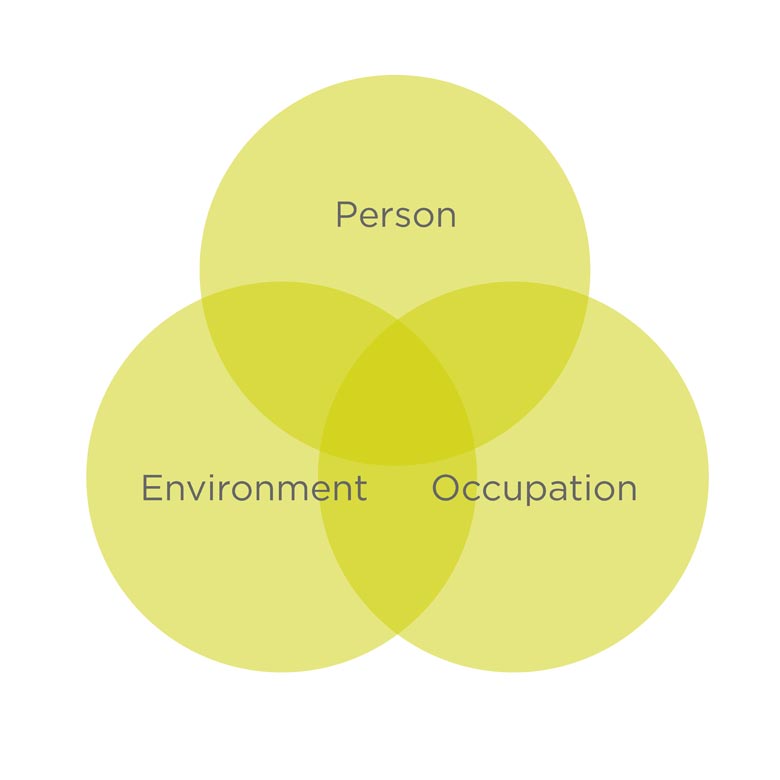
Occupational therapists often use a model or conceptual framework such as PEO to clearly understand the complex relationship between all aspects of the individual and determine an appropriate occupationally focused therapy plan. This is no different with the occupation of bathing.

However, bathing assessments have largely become about the physical transfer rather than being occupation focused.
Determining how someone accesses the bath is very different to why someone accessed the bath.
Consider this question:
Why do you bathe?
Generally, the answer is related to relaxation, play (for children) or role reinforcement (parents or carers). Rarely do people use a bath specifically to become clean. This is simply a by-product of accessing the bath – you do it while you’re in there.
On that basis do you ask your clients that question or are you conducting a transfer assessment?
Without asking ‘Why?’ it is unlikely that you have been able to gather all of the information required to make a client centred, holistic and occupational focused recommendation. This is often the missing reasoning when making the leap from bathing to showering.
Consider how you determine the complex relationship between person, environment and occupation without knowing what the person finds meaningful. This omission might lead to an assumption that the focus is hygiene which leads to the recommendation of a level access shower for example. However, consider the impact on long-term wellbeing if other meaningful occupations were inhibited by that recommendation, simply because we asked (or looked for) ‘how?’ and not ‘why?’.
Practicing occupational therapy must be about the ‘why?’ to ensure it supports engagement in meaningful activity.
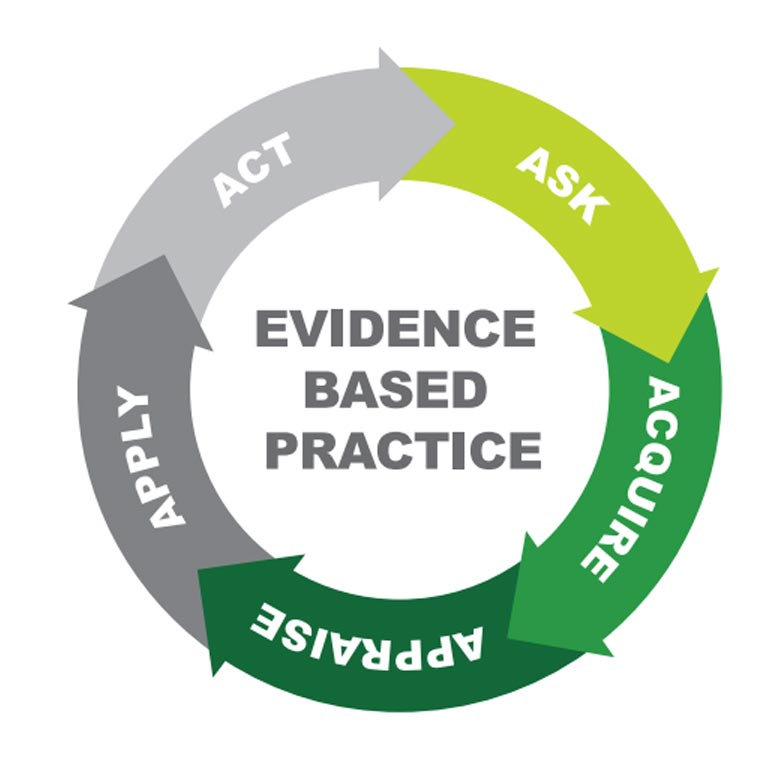
Research
Robust clinical reasoning relies on use of the most up-to-date evidence base. This evidence base includes relevant research that can be applied to ensure recommendations are defensible.
However, are occupational therapists generally comfortable and confident in sourcing and applying research to their daily practice?

On the subject of bathing there is significant research on benefits to:
- Sleep
- Skin cleansing
- Circulation
- Muscle healing
- Mental health and well-being
Although the majority of therapists are likely to be able to identify these rhetorically, it is important to understand the research so that the evidence can be accurately applied to practice.
As an example, let’s look at bathing and the impact on sleep; what does the research say?
- Murphy (1997) & Kanda (1999) conducted studies that, through physiological testing, demonstrated improved sleep following bathing.
- The University of Texas (2019) completed a systematic review of over 5,300 sleep and water-based studies, concluding that bathing had the biggest impact on the circadian process. More than that, they were able to determine when a bath should be taken and at what temperature to optimise sleep.
Consider the possibility of being able to positively impact on sleep and the impact that could have on the client, their family or their carers.
From an occupational perspective there is then a large bank of research that supports the benefit of sleep in these areas:
- Education
- Behaviour
- Physical health
- Mental health
- Play
Part of a robust clinical reasoning process is the ability to apply the evidence to maximise outcomes. If, for example, a recommendation was to replace a bath with a level access shower because of complex transfers, would the therapist consider the potential impact of this on the above research areas?
It is important that in ensuring recommendations are defensible and clinically reasoned, that the therapist has all required information to formulate a client centred, holistic and occupationally focused plan. This includes information about the person, their environment and their meaningful engagement in occupation, supported by the most up-to-date and relevant evidence base.


For a pdf of this information and a CPD certificate click here.
For bespoke CPD education or any queries,
call the Abacus Academy on:
01527 400024

